Shop Now /
FloraBoost
Sku: 859051

The strains of probiotic bacteria in FloraBoost have been strategically selected based on research which supports their survivability and adherence to the intestinal tract. FloraBoost comes in a powder form for easy administration to children.
Categories:
Immune Health, Springboard (Kids), Gastrointestinal Health
Clinical Applications
- Helps Maintain Gastrointestinal Balance in Children
- Increases Secretory IgA for Enhanced Gut Immunity
- Supports Bowel Regularity
- Supports Digestion and Micronutrient Absorption
The gastrointestinal (GI) tract is a finely balanced environment where roughly 500 different strains of bacteria compete for space and nutrients. The natural microflora balance can be disrupted by medications, such as antibiotics, or poor dietary intake. One of the key benefits of probiotics is their ability to increase populations of healthy bacteria in the face of microflora imbalance. In addition, extensive research has identified other broad health benefits, including supporting healthy bowel function, increasing the production of important short-chain fatty acids that provide energy to the cells of the intestinal lining, boosting immune function, aiding in the digestion of difficult-to-break-down compounds like lactose and casein, and enhancing detoxification of harmful compounds.
Because probiotics are living organisms, there are various challenges associated with their manufacturing and distribution. For a probiotic to be effective, it must be shelf-stable through the expiration date and precisely delivered to the intestinal tract, where it can have maximum benefit. The microorganisms in FloraBoost are protected, sealed, and freeze dried away from moisture, heat, light and oxygen. This allows the bacteria to remain dormant until they are exposed to moisture in the GI tract.
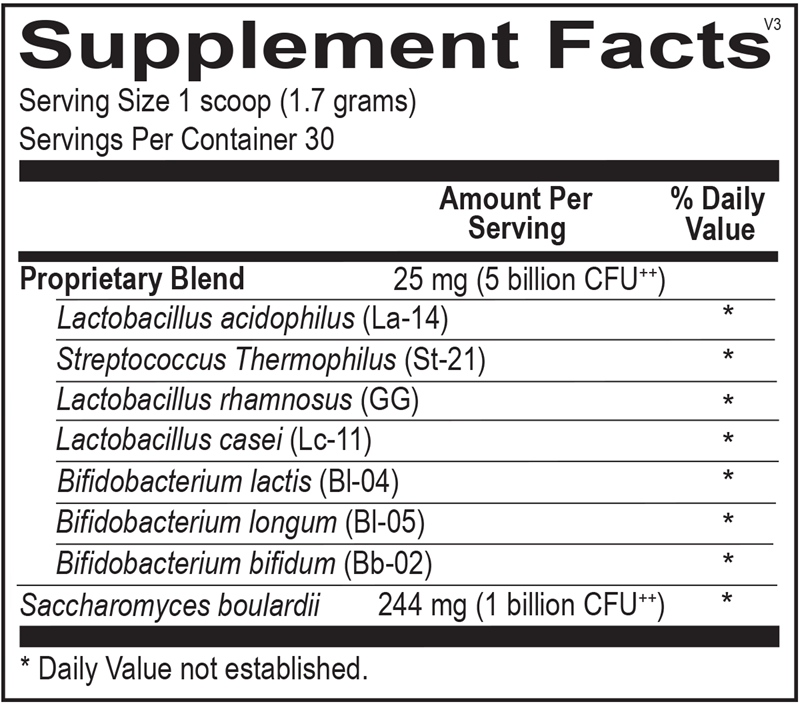
FloraBoost is a probiotic formula for children, designed to deliver live bacteria that promote healthy gut microflora, protect intestinal integrity and boost immune function. The formula contains three strains of Lactobacilli and three strains of Bifidobacteria, as well as Streptococcus thermophilus and Saccharomyces boulardii, an extensively researched microorganism shown to help restore microflora balance by enhancing commensal organism function. The eight strains in FloraBoost have been strategically selected based on research supporting their survivability and adherence to the intestinal tract. FloraBoost comes in a powder form for easy administration to children.
Suggested Use:
Add one scoop (1.7 grams) to a glass of water or the beverage of your choice, stir and drink, or as recommended by your health care professional.
Lactobacillus acidophilus (La-14)
Lactobacillus acidophilus is a beneficial bacteria strain that is normally found in the intestinal tract and mouth, and is commercially used in dairy products for the production of acidophilus-type yogurt. L. acidophilus ferments various carbohydrates to produce lactic acid, which increases the absorption and bioavailability of minerals, including calcium, copper, magnesium and manganese. The production of lactic acid also promotes health by creating an inhospitable environment for invading microbes. L. acidophilus has been shown to protect intestinal cells by competing for adhesion space in the gut against harmful bacteria. The L. acidophilus strain in FloraBoost has been specifically chosen because of its strong adherence and survival attributes in the GI tract.
Bifidobacterium bifidum (Bb-02)
Bifidobacterium bifidum is a normal resident of healthy infant GI tracts and usually colonizes within four days of life. It has been shown to effectively compete with harmful bacteria, which suggests B. bifidum’s lactic acid and acetic acid production provides an antagonistic action against pathogens to help maintain microflora balance.
Lactobacillus rhamnosus (GG)
Lactobacillus rhamnosus has been frequently used in the prevention and treatment of occasional diarrhea in children. L. rhamnosus has also been shown to promote GI health by increasing intestinal cell replication.
Streptococcus thermophilus (St-21)
Among 80 infants, 6-36 months old, with occasional diarrhea, given either a formula supplement with Bifidobacterium lactis and Streptococcus thermophilus or non-supplemented formula, those receiving the probiotic formula had fewer incidences of diarrhea. A second study of 80 breast-fed children, 6-24 months old, with occasional diarrhea for fewer than four days, found those given either a yogurt containing S. thermophilus and L. bulgaricus had shorter hospital stays, better weight gain and reduced loose stool frequency.
Saccharomyces boulardii
Saccharomyces boulardii is probiotic yeast that was first isolated from the skin of the tropical fruits lychee and mangosteen in 1923 by French scientist Henri Boulard, following the observation that mangosteen consumption controlled occasional diarrhea in natives of Southeast Asia. S. boulardii plays a role in supporting immune defense by increasing levels of a crucial antibody, sIgA, and creating a first line of defense that helps bind and clear harmful bacteria.

Related Products
FloraBoost
Sku: 859051
The strains of probiotic bacteria in FloraBoost have been strategically selected based on research which supports their survivability and adherence to the intestinal tract. FloraBoost comes in a powder form for easy administration to children.
Categories:
Immune Health, Springboard (Kids), Gastrointestinal Health
Clinical Applications
- Helps Maintain Gastrointestinal Balance in Children
- Increases Secretory IgA for Enhanced Gut Immunity
- Supports Bowel Regularity
- Supports Digestion and Micronutrient Absorption